Day 2 :
Keynote Forum
Kumale Tolesa Daba,
Jimma University, Ethiopia
Keynote: Bilateral keratomalacia secondary to diet induced vitamin A deficiency in an Ethiopian young woman: A case report

Biography:
Kumale Tolesa Daba has completed Doctor of Medicine degree from Jimma University, School of Medicine and Ophthalmology specialty. She is an Assistant Professor
of Ophthalmology in Jimma University. She has published 4 papers in reputed journals and has 6 more pending publications. She has inclination towards Glaucoma and
Pediatric Ophthalmology. She did a short term fellowship on Pediatric Ophthalmology and strabismus at Gachon University Gil Hospital, South Korea and Tilganga Institute
of Ophthalmology, Nepal.
Abstract:
Diet induced vitamin A deficiency is less commonly seen in otherwise healthy adults, due to large store of vitamin A in the
body. Night blindness is the commonest manifestation of vitamin A deficiency in adults, whereas keratomalacia is a rare
manifestation. A 27 years old Ethiopian woman came to Jimma University Department of Ophthalmology with a compliant of
protrusion of the globe content of both eyes within a week, after having redness and fear of light of both eyes for 2 months. She
is a mother of twins and has low socioeconomic status. On general examination she is catechetic with enlarged parotid gland.
On ocular examination she is bilaterally blind and has dry ocular surface. There was bilaterally melted cornea with prolapsed
uveal tissue. After going through several investigations, she was diagnosed as bilateral keratomalacia (stage X3B) secondary
to diet induced vitamin A deficiency. She was supplemented with vitamin A and other nutritional supplementation. Topical
lubricating drops and ointments were administered. Finally conjunctival flap was done to preserve the globe. Although it is
rare, treating physicians should be aware of the occurrence of keratomalacia in adults which is potentially blinding. Early
recognition and treatment of vitamin A deficiency at the stage of night blindness is very essential in reducing blindness caused
by keratomalacia.
- Innovations in Optometry | Imaging Techniques | Ophthalmic Instruments | Visual Optics
Location: Paris

Chair
Juan Bolívar Parra
DO-FIAO, Spain
Session Introduction
Rohit Sharma
Burton Hospitals NHS Foundation Trust, England
Title: 24 hour IOP monitoring –concepts & an overview including Triggerfish

Biography:
Rohit Sharma a consultant Ophthalmic surgeon working in NHS England. Received Clinical Excellence Awards from the NHS trust for his contributions & received Fight For Sight Award by the Royal College of Ophthalmologists London. Examiner for the FRCS Exams for the Royal College of Surgeons Edinburgh Represents Royal College of Ophthalmologists London for conducting Consultant interviews. Interviewer for University Medical School & doctor recruitment in the NHS. Led "Listening in Action" work in the NHS UK, is a certified Quality Service Improvement & Redesign Practitioner, completed "True Leader" workshops & is a certified Risk Assessor. Investigation officer for significant adverse events & is on the teams for service improvement & business planning.
Abstract:
Intraocular pressure (IOP) is still one of the most important modifiable risk factors for glaucoma progression. Hence naturally,
the measurement, monitoring of IOP & its lowering by various methods (surgical, medical, laser) remains the mainstay
of effective management of this potentially blinding chronic condition. Goldmann applanation tonometry remains the gold
standard but a single IOP measurement in the clinic during office hours cannot account for the diurnal variation, nocturnal
IOP profile & postural variations which have all been found to be important. Though many of these need development, the
developments are exciting. Triggerfish (Sensimed), a contact lens sensor (CLS) is an exciting & innovative device to monitor
the 24-hour IOP. Though there are some inherent assumptions and limitations of this technology, the potential, safety and
reproducibility profile is very good. I have led the successful setting up of the first triggerfish centre in NHS England along
with my team. The potential advantages as well as the limitations of this triggerfish technology & the other methods/attempts
to address this unmet of 24 hour IOP monitoring will be discussed.

Biography:
Juan Bolívar Parra received a Doctor of Osteopathy (DO) degree from the University of Granada (1997). He is a Fellow of International Academy of Orthokeratology and Control of Myopia (IAOMC) in Budapest 2015 and member of Eurok since 2012. He is a Member of the Board of Spanish Section of the IAOMC. He is a Professor of the Master's Degree course in Clinical Optometry and Advanced Optics at the University of Granada. He had conducted over 70 graduate courses, including Course in Advanced Clinical Optometry (UEM). He has participated with papers and posters in different congresses (Eurok Budapest 2015, SAO 2016, Optom 2016, Eurok Iberica Granada 2016). For 14 years, he has run his own center in Alcalá la Real-Jaén (Centro Óptico Real). His areas of specialization are advanced contactology, especially ortho-K, highlighting for being able to customize the adaptations to be successful in cases that were previously not viable.
Abstract:
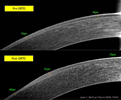
In this talk, there will be an update in Ortho-K, showing the mechanisms of action of the lenses and how the hydrodynamic
forces occur between lens and cornea work. It will be shown that it does not just work by pressing on the apex. The periphery
is even more important. The changes produced after Ortho-K in the corneal epithelium will be shown through OCT images
of real cases. The risks presented by this technique will be assessed. All current applications of Ortho-K will be exposed, not
only myopia, assessing which patients can be applied at present and which refractive defects can cover, as well as where the
Dp limits are currently. Special emphasis will be placed on the control of myopia in children, comparing it with other options,
based on the scientific evidence published. Finally we will give pearls of how we can customize the adaptations in children, in
order to optimize myopia control.
Shroug M Aldaham
Complutense, Ministry of Education, Saudi Arabia
Title: Visual field changes in type 2 diabetics without retinopathy: A review

Biography:
Shroug Aldaham has recently graduated from Complutense University of Madrid (UCM),Spain with a PhD degree in Optics, Optometry and Vision. She has aBSc (Hons) inOptometry from King Saud University (KSU), Riyadh, Saudi Arabia, and a Master of Science in Vision Science from the University of Waterloo,Ontario, Canada. She has joined the Optometry department at KSU as a demonstrator (an academic position that prepares for professorship) before joining the Master program in Canada. After her masters she returned to Riyadh and later joined the PhD program at UCM. Both of her Masters and PhD studies were Saudi government-funded research grants. She has a research experience in pediatric vision screening and visual function testing in diabetics and has published in international optometric and vision research meetings. Her research interests are pediatric and diabetic visual.
Abstract:
Background: Diabetic retinopathy (DR) progression has a direct effect on vision, which by time will cause visual deterioration.
(1) Localized visual field (VF) sensitivity losses were reported in diabetics with background DR and clinically significant
macular edema.(2,3) There is little information however about VF changes in diabetics without retinopathy.
Purpose: To review VF changes in diabetics without retinopathy.
Methods: A literature review was conducted on testing VF in diabetics without retinopathy. The search criteria considered the
type of diabetes, the type of VF stimulus presented, and the instrument used.
Results: The source of variability in the VF results in diabetics depended on the difference in the instrument and/or stimulus
used, as VF changes were reported for some instruments while others did not report any change. (i.e. whether it was standard
automated perimetry, short wavelength automated [blue-yellow] perimetry, or frequency doubling [FDT] perimetry).
Differences between type 1 and type 2 diabetics were also reported. When compared to type 1 diabetics, few studies have tested
type 2 diabetics without retinopathy.


Conclusions: Care should be taken when comparing VF changes between studies related to the type of diabetes, type of
stimulus and instrument used. This presentation will further elaborate the differences between VF tests. Also, clinical VF data
for type 2 diabetics without retinopathy will be presented; aiming to see if VF testing can be used as a clinical screening tool for
type 2 diabetics before retinopathy is detected.
- Retina | Cornea | Orthokeratology and Orthoptics
Location: Paris

Chair
Rohit Sharma,
Burton NHS Foundation Trust, England
Session Introduction
Rohit Sharma
Burton Hospitals NHS Foundation Trust, England
Title: Laser and surgical management of glaucoma-A current overview

Biography:
Rohit Sharma a consultant Ophthalmic surgeon working in NHS England. Received Clinical Excellence Awards from the NHS trust for his contributions & received Fight For Sight Award by the Royal College of Ophthalmologists London. Examiner for the FRCS Exams for the Royal College of Surgeons Edinburgh Represents Royal College of Ophthalmologists London for conducting Consultant interviews. Interviewer for University Medical School & doctor recruitment in the NHS. Led "Listening in Action" work in the NHS UK, is a certified Quality Service Improvement & Redesign Practitioner, completed "True Leader" workshops & is a certified Risk Assessor. Investigation officer for significant adverse events & is on the teams for service improvement & business planning.
Abstract:
Glaucoma is a slow insidious sight threatening condition which can potentially cause irreversible visual field loss and blindness. Successful treatment is imperative after timely detection and monitoring. Current management usually starts with ocular hypotensive agents (eye drops) which need regular compliance and can have local and systemic side-effects. Laser
management includes laser trabeculoplasty (argon and selective) for open angle glaucoma, peripheral iridotomy for angle closure and iridoplasty. Cyclodiode laser is used for nonseeing eyes, intractable glaucoma and also in seeing eyes in certain conditions. Trabeculectomy filtration surgery with antimetabolites is still the gold standard invasive surgery. There are specific indications for glaucoma drainage implants like tubes. Recent advances include minimally invasive procedures like XEN, Istent which have their place in the armamentarium. An overview of the various laser and surgical options of glaucoma management for a general ophthalmologist, optometrist and general practitioner perspective shall be presented by a practicing glaucoma
surgeon.
Nuha Fath Elrahman
Al-neelain University, Sudan
Title: The impact of Rose -K RGP contact lens wear on the visual performance of keratoconic eyes

Biography:
Nuha Fath Elrahman obtained PhD in Optometry and Visual Science in 2009. She started the Department of Medical and Ophthalmic Photography and is the
Head of the Department of Medical and Ophthalmic Photography at Al-Neelain University, Sudan. She is a Member of Al-Neelain University Senate and General
and Academic Secretary of Sudanese Union of Optometrists. She is a Member of the Medical and Health Professional Council and AOA, and attended many
international conferences.
Abstract:
Aim: The study was designed to be a comparative cross sectional study. It was aimed to evaluate the effect of rigid gas permeable
contact lense wear (Rose-k menicon) on visual performance (vision, color vision and contrast sensitivity) in keratoconic
patients with different degree of keratoconus. Material and method: The history of the patients was taken to be sure that the
patient have no history systemic and ocular diseases, the corneal curvature was measured by auto refkratometer (Nidek)
to determine the degree of KC, the vision was tested by Snellen´s test type (E-test). Refraction was done subjectively using
(stenopic slit), Rosek2 lenses (menicon) was use to correct refractive sate of the eye, the color vision was evaluated with
(Ishiaraa) test and contrast sensitivity with (low contrast slip Thark), these measurements were taken with and without Rose
k2 contact lens. Results: The data were analyzed using SPSS program and the following results were obtained: A total number
of 50 patients (100 eyes) were found to fulfil the criteria of selection (31 males and 19 female) their ages were ranged from
10 - 35 years with a mean of (22.72 years ±5.79). Ninety four percent of the patients had moderate (52%) to sever (42%)
keratoconus. Their base line vision ranged (1/60-6/9) with mean of 0.10±0.10, 99% of them less than 6/18, and with rose-k 2
contact lens was from (6/12 to 6/6 ) 97% their vision was within the normal limits from (6/9 to 6/6) with a mean of 0.88±0.20,
Independent t-test showed significant differences base line and with rosek2 P value 0.000 . The base line color vision showed
that 62% of the patients showed abnormal color vision and Chi-squire test yielded a significant difference between base line
color vision and color vision with contact rose -K CL P value 0.016. The base line contrast sensitivity ranged from 0.5 to 125
with mean of 1.08±0.14. 62% of the patients showed abnormal base line contrast sensitivity compared to 100% of normal
contrast sensitivity with rosek2 mean 1.25±0.00. Paired sample t-test showed a significant difference between baseline contrast
sensitivity and after wearing rose K contact lens P 0.000.
Conclusions: Rose -K RGP contact lenses significantly improve the visual performance